SURGICAL ADVANCEMENTS IN UROLOGY
Little Things Make a Big Difference
Have you hugged your urologist today?
If you’ve ever found yourself in need of this kind of specialist, chances are they are at the top of the ‘hug’ list. That’s because suffering with a challenge ‘down there’ is, at best, annoying and at worst, debilitating.
Urology is a medical specialty that addresses diseases and complications that compromise the good-working order of the organs of the male and female urinary tract including the kidneys, uterus, bladder and urethra. Urologists are also medical specialists in the male reproductive organs (testes, prostate and penis). Being able to access advanced care within the specialty is absolutely critical as it can have a significant impact on one’s quality of life.
Ask any Kelowna General Hospital (KGH) urology patient and they will tell you, the urologists at KGH are second to none. Since 2021, KGH has been home to Dr. Jennifer Locke, a brilliant urologist with subspecialty training in reconstructive urology. Soon after her arrival, Dr. Locke noted that a critical piece of equipment could make a big difference for her team and their patients.
From sinuses to arteries to urethras, abnormal narrowing or constriction of a body passage is generally not a good thing. The urethra is a tube that carries urine from the bladder so that it can be expelled. Narrowing of the urethra restricts this flow and can cause a variety of medical problems in the urinary tract, including inflammation or infection. Narrowing in the male urethra is known as a male urethral stricture and if left untreated, can cause serious problems including bladder and kidney damage and infections caused by the obstruction of urine flow.
When Dr. Locke joined the KGH urology team, patients in the southern interior of BC with symptoms of urethral stricture were referred to the Lower Mainland for diagnosis and treatment.
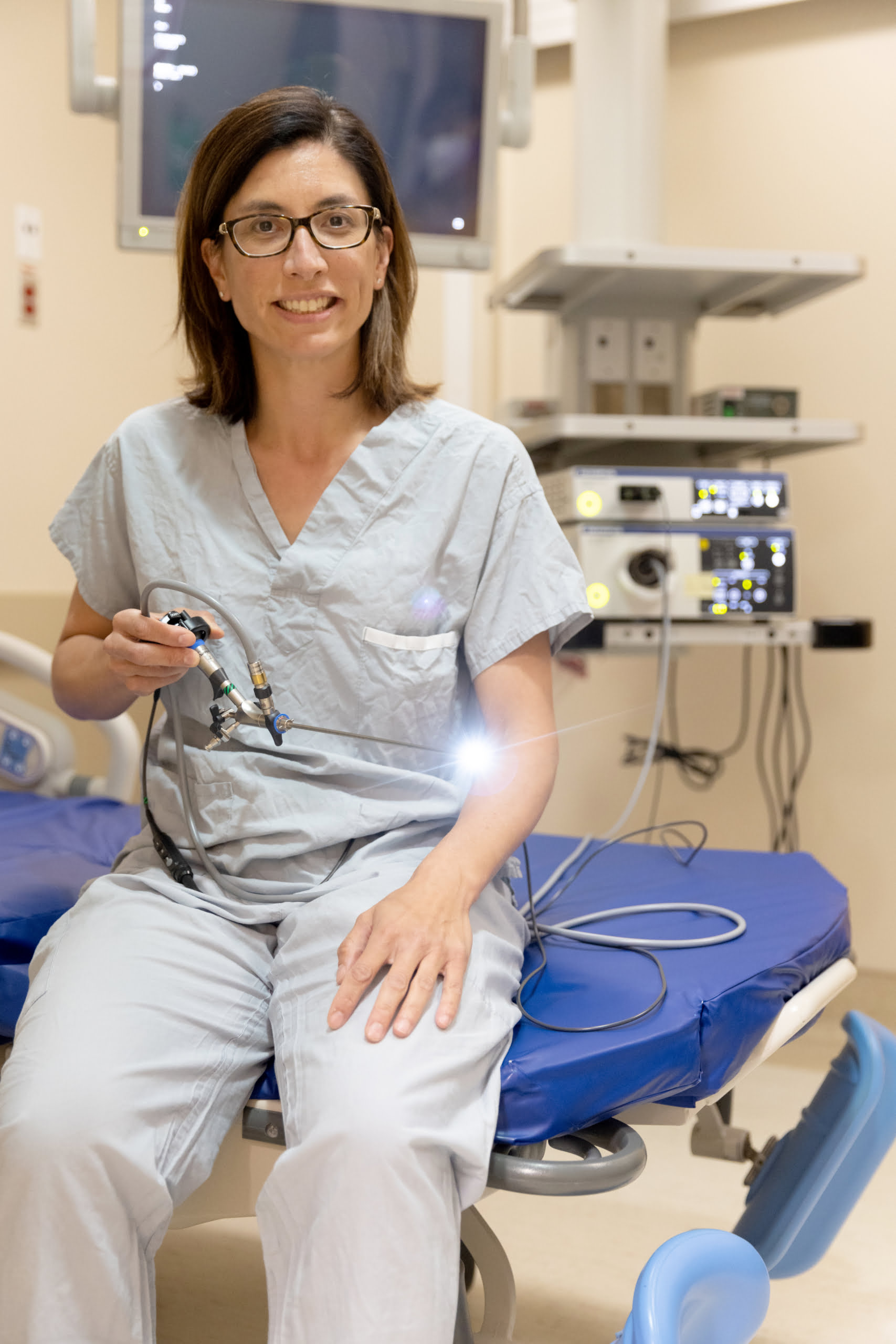
Dr. Locke reached out to the KGH Foundation seeking funding for several pediatric (referring to the size) cystoscopes – diagnostic tools so small they can be inserted into a 6-8 mm tube, the diameter of the average male urethra. Acquiring these special scopes would allow KGH urologists to diagnose the length and calibre of the stricture and avoid sending patients to the Lower Mainland.
Last year, a significant estate endowment to the KGH Foundation provided the funding required.
“The utility of having access to these pediatric cystoscopes is immense,” states Dr. Locke. “I am now equipped to do the appropriate work-up and all types of surgical treatments for men from across the Interior Health region. This absolutely improves patient comfort and urethral repair outcomes.”
Dr. Locke explains, “Two of my patients had been in and out of the hospital with UTIs (urinary tract infections) and sepsis, secondary to urethral strictures. One of them developed endocarditis and the other had life-threatening heart arrhythmias triggered by episodes of sepsis. Because we were able to accurately diagnose the urethral strictures here at KGH, in both cases, we performed urethroplasty (surgery to repair a urethral stricture) and my patients have been infection free since.”
Since acquiring the cystoscopes, Dr. Locke and her team have diagnosed and performed urethroplasty on dozens of patients, many from out of town, not only improving the quality of life for these patients but also allowing them to stay closer to home for treatment and avoiding travel and accommodation costs to receive care at hospitals in Vancouver or Calgary.
“Our patients have told us that they feel like their life has been given back to them after urethroplasty surgery,” shares Dr. Locke. “They are grateful that they don’t have to live with tubes in their bellies or urethras, which makes for a significant quality of life improvement. And I am forever grateful for this support and look forward to serving my community.”